


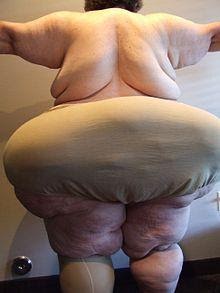

Images from: https://en.wikipedia.org/wiki/Lipedema
This is not the image of service user but of an example the medical condition.
The service user presented as a bariatric service user, however due to severe lipolymphedema syndrome, the service user had extensive oedema on her legs and hip area resulting in very large overhang at each side of her body at hip level.
This presented a unique situation when sourcing solutions to support the service user with mobility and moving and handling solutions.
The service user lived in a mid-terraced house with her daughter; at the rear of the property the ground floor there has been an extensive adaptation to support the service user.
The service user was supported at home for activities of daily living and personal care; this was facilitated by her daughter.
At the time of assessment the service user reported that she could get up from her bed and was currently using the commode as a standing frame, her daughter stabilised the commode by sitting on it. Using the commode in this way is not fit for purpose and in time would cause stresses on the material and structure of the commode.
The service user stated once in standing she could take some steps with the support of a walking frame to her wet room area. This was not observed at the time of the visit.
The service user had a fall withing the last year and had subsequently had another fall at home post this visit; both falls resulted in the service user being on the floor for a considerable amount of time while emergency services supported her from the floor back to bed.
As stated previously the system in place to support the service user into standing was not fit for purpose. It was strongly recommended to ascertain the actual functional ability of the service user in relation to her weight bearing and walking ability. This will ensure that all equipment currently provided was fit for purpose.
It would be beneficial for the service user to have different systems in place for when she is feeling at her best, when she is able to stand and step and an alternative system for when she is able to stand but not self-transfer. Both would require a full assessment due to the service users body shape and medical condition.
At the time of the visit the service user had a good range of movement of her upper body and was able to move her legs laterally in the bed, she was not able to roll or turn. The Tissue Viability Nurse stated that the service user was unable to roll or turn due to her medical condition. The Tissue Viability Nurse also stated that to facilitate a roll or a turn with the service user would have a negative impact on her health and wellbeing.
Long flat slide sheets could be used to eliminate the need of turning or rolling the service user. It was strongly recommended to support any insertion of emergency equipment or hoist slings using the method of folding the slide sheets and unravelling them under the service user.
The bed is designed to come into a seated position for front access and egress. The service users feet were pressed against the foot plate which had no pressure relieving qualities and had been modified with dressings to provide a non-slip surface for when the service user stands
The bed was not height adjustable; this would impact greatly on care being facilitated in the bed and pose a significant risk to any carers as they would not be able to adopt the correct postures for facilitating safe moving and handling.
The service user reported there were some maintenance issues in relation to the mattress and the mattress provided did not support in the management of moisture. Although this is not within the remit of the assessment for moving and handling, it was strongly recommended to source a mattress that facilitates microclimate management and effective pressure relief, as the current mattress did not appear to be meeting the needs of the service user.
The service user was at risk of falling and required systems in place to support her when a fall occurs. With the implementation of a system to support the service user from sitting to standing as identified earlier this may reduce the risk of falls.
However, a coordinated approach is required to support the service user when she falls. The Mangar Camel may support the service user if she is able to assist. The Mangar Camel can be placed under the service user by using 2 flat slide sheets and sliding the device between the slide sheets.
For times when the service user is unable to maintain a sitting posture or needs to be evacuated from the house into an ambulance it is recommended using the Hover Jack in conjunction with the Hover Mat for safe lateral transfer onto the bed or trolley.
This device is placed under the service user by inserting it between 2 flat slide sheets already placed under the service user. At floor level this can be a difficult technique to undertake and will require practice as well as a coordinated approach.
The service user did not have a hoisting system at home. It was strongly recommended that due consideration was given to the long-term care needs of service user and therefore planning for supporting with hoisting is implemented at this stage.
An XY system will eliminate the need to consider other methods identified for retrieval from the floor in the event of a fall, as the service user would be able to be hoisted from the floor.
Report completed by:
Janet Brooks,
Senior Manual Handling Advisor,
30th April 2015.
Date of action: ASAP
Objective:
To flat lift the service user on her current mattress system to enable TVN (Tissue Viability Nurses) to visually access and check Sacral area for possible tissue damage.
Process:
The task will be to:
On completion reverse the process removing Hovermat slings first then slide sheet. Return bed mattress to preset pressures. Reposition service user.
Manual Handling adviser to practically demonstrate process in training environment with all relevant staff required for this task.
A bariatric suit shall be used to facilitate reality of shape and size, it must be stressed this will not replicate the true weight of the service user.
Completed by:
John Humphray
Manual Handling Trainer, Bariatric Handling Specialist
Date of transfer: 15th June 2015
A process was required to transfer this service user as this situation had become a safeguarding issue and it was a matter of urgency that this service user be transferred onto a safer system while a review of her care plan and long term care be established.
Objective:
To move the service user from her current failing bed and mattress onto an interim surface while the bed and mattress were replaced with a new system.
The task was to laterally slide the service user onto the interim surface then back onto the new surface provided. The actual technique and equipment to be used were to be identified on the day following a dynamic risk assessment of the needs of the service user, the environment and any other associated risk factors. These were communicated to the lead occupational therapist at all times during the task. The moving and handling advisor on site gave full and clear instructions to the team and no activity was undertaken without full consent of the service user.
If at any time it was deemed the health of the service user was at risk from being moved the task would be stopped and the GP or emergency services contacted.
Onsite assessment:
The service user currently used a bespoke designed bed and a partial low air loss mattress. The top half of the mattress is a air system which is joined at the bottom half with a static softform surface.
The bed is not height adjustable; this impacts greatly on care being facilitated. It was observed that the daughter needed to go down on her knees to facilitate any moving of the lymphedema at the hip area. This poses a significant risk to any carers as they would not be able to adopt the correct postures for facilitating safe moving and handling.
The bed was designed to come into a seated position for front access and egress. The point at which the mattress membrane joined had split and was pushed down into the bed frame.
The service user stated that part of her sacral area was stuck in this membrane, that the area felt numb and was difficult to move.
She stated to move this area she profiled the bed into a flat position and by forcing her feet against the footboard of the bed frame, pushing up, was sometimes able to release the pressure in this area. This was becoming more painful and difficult to achieve.
The daughter stated her mother had fallen some 10 weeks earlier and since then had not moved from this bed.
The service user had a good range of movement of her upper body and was able to move her legs laterally in the bed, she was not able to roll or turn.
Due to severe lipolymphedema syndrome, the service user had extensive oedema on her legs and hip area resulting in a very large overhang at each side of her body at hip level.
At the time of assessment it was asked if anyone had been able to see the area of sacral that had been trapped inside the mattress membrane, the answer from all was no.
The environment was cluttered and, at the time of the visit, estate teams were expanding the front door width.
It was agreed by all that a meeting should take place to discuss the options available to facilitate a safe transfer of the service user. It was also important that the daughter, attend this meeting.
A discussion took place to assess that the equipment proposed to be used and handling techniques presented were suitable.
The plan was to laterally transfer the service user onto a new bed surface built alongside the current system. This would be facilitated by the use of a Hovertech 39” Hovermat sling. A demonstration of this equipment was presented at this meeting
This system is air operated and can reduce the weight of the service user from 100% to 17%, significantly reducing the risk of injury to both service user and supporting staff. This system would also enable the sacral area to pop out gently with reduced risk of further damage.
It was not possible to insert large slide sheets as the sacral area was trapped inside the membrane of the mattress falling through the bed frame.
It was stated that it was necessary to prepare the emergency services in case there was an issue such as an arterial bleed in the sacral area. No one knew whether or not there was already significant damage as no one had seen this area for some time.
No activity was undertaken without full consent of the service user. It was agreed that all would be explained to the service user including the possibility that she may have to be removed to hospital.
All agreed that the daughter and senior OT’s would explain this to the service user.
Plan of action:
Technique:
The above action was completed safely, however, a flat slide sheet was now able to be placed safely under surface user on the new surface to enable better repositioning.
Clinical nursing staff then assessed damaged skin area and re-dressed.
It was not possible to get right under the sacral area due to the body mass pressure on the mattress surface.
It was agreed that the service user had had enough and needed to rest, a further plan would be discussed at a future M.D.T. (Multidisciplinary Meeting) including the best way forward to support the service user and daughter.
Completed by:
John Humphray
Manual Handling Trainer, Bariatric Handling Specialist
